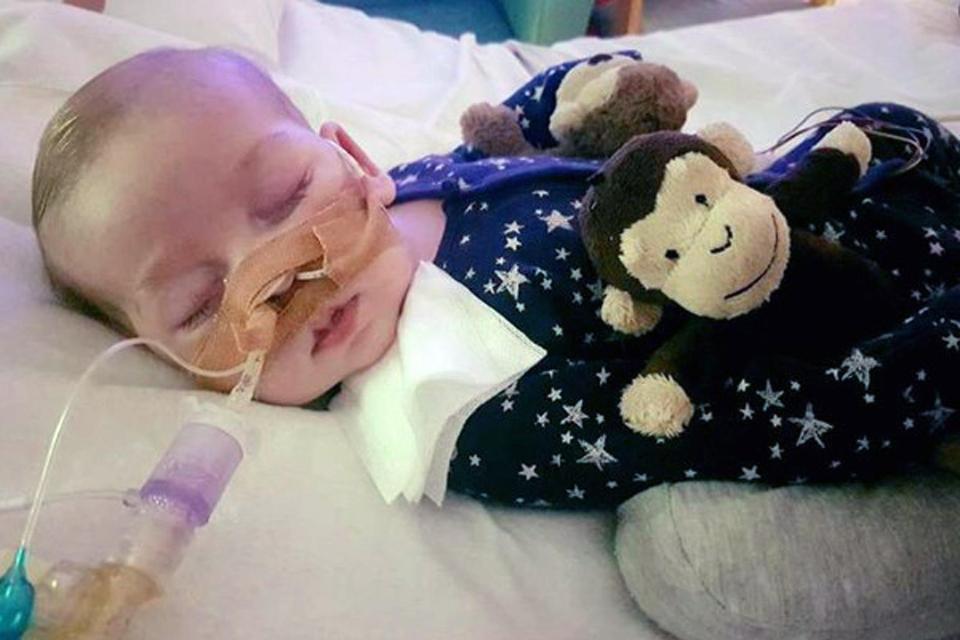
Charlie Gard saga may end in days
The European Court of Human Rights is considering whether to to allow the withdrawal of treatment.
The protracted legal saga surrounding 10-month-old UK infant Charlie Gard, who suffers from a rare genetic and has brain damage, may come to an end in days. The European Court of Human Rights (ECHR) is currently considering whether to affirm the decision of UK courts to allow the withdrawal of treatment.
Gard suffers from mitochondrial DNA depletion syndrome, and has been on life support for several months in Great Ormond Street Hospital for Children, London. In early April the High Court in London ruled that it was in Gard’s best interests that treatment be stopped and he be allowed to die. His parents have attempted, unsuccessfully, to appeal against the decision. Gard’s parents want him to be discharged from Great Ormond Street to travel to the US for an experimental treatment known as nucleoside replacement therapy.
The ECHR – the last court of appeal for the Gards – says it is currently considering written submissions, and has asked the Hospital to maintain life support until midnight next Tuesday.
The case has divided ethicists in the UK, with some arguing that it would be “reasonable” to allow Gard to be taken to the US for treatment.
Writing recently in The Lancet, Oxford bioethicist Julian Savulescu challenged the reasoning behind the High Court decision:
The claim that Charlie Gard’s life is objectively against his best interests turns, crucially, on the claim that a very small chance of a small improvement is outweighed by the suffering attending his condition and its treatment. But this not an “objective fact” but a value judgment. There is space for reasonable disagreement. For example, is a one in 10000 chance of improvement worth some months of “unpleasantness”, of needles and invasive procedures?
In a response to Savulescu, Oxford neonatologist and bioethicist Dominic Wilkinson disagreed:
…a shift in perspective casts that argument into doubt…imagine that there were a sudden epidemic of mitochondrial DNA depletion syndrome affecting thousands of newborn babies. Would it be ethical to artificially ventilate for months thousands of infants to achieve some measure of improvement in one infant? … it seems wrong to subject thousands of infants to invasive and unpleasant life-support treatment to benefit one child. That implies that this chance of recovery is too slim to make treatment plausibly in the current child’s interests.
Charlie Gard saga may end in days
Xavier Symons
Creative commons
https://www.bioedge.org/images/2008images/Charlie_Gard.jpg
medical futility
neonatal care
uk
withdrawal of life support
- Can machines be moral? - March 7, 2021
- Can we synthesise Christianity moral theology with secular bioethics? - November 28, 2020
- Euthanasia polling data may fail to capture people’s considered views - August 15, 2020
